
By Randall Zarin, MBA, MPH, CPA
Medical schools and teaching hospitals share an intertwined relationship that not only shapes the future of healthcare but also plays a significant role in the economic sustainability of both institutions. Clinical faculty members from medical schools, working as physicians at teaching hospitals, contribute in several ways, from patient care to medical research, and additionally, through their educational responsibilities. Understanding how these contributions generate financial value, drive growth, and ensure long-term sustainability is key to the partnership’s success. Determining the economic contribution, an analysis of the value of services that an entity provides another, is a beneficial exercise to determine how the clinical faculty benefits the teaching hospital, and how the teaching hospital benefits the tripartite mission of the medical school.
This analysis illustrates the absolute importance of the economic contribution of the medical school faculty to their teaching hospital. Their clinical services generate substantial revenue, their research fosters innovation and external funding opportunities, and their educational efforts ensure a pipeline of both skilled physicians who contribute to the hospital’s long-term success, as well as physicians-in-training (residents; fellows) who maintain 24/7 oversight of patients. Without this academic partnership, the hospital’s ability to maintain its competitive edge, sustain itself financially, and fulfill its mission would be significantly compromised as will the ability for the medical school to train physicians for the benefit of the community. Clinical faculty’s presence impacts the hospital in several key ways:
- Higher Acuity and Specialized Care: Medical school faculty are typically experts in their fields, and they often handle the most complex and high-acuity cases. This not only improves patient outcomes but also drives the hospital’s reputation for excellence. Specialized care attracts more patients, leading to increased revenue streams and higher reimbursement rates from insurance companies.
- Quality of Care and Continuous Improvement: Medical faculty bring with them cutting-edge knowledge, which helps in the continuous improvement of patient care. Their involvement in research and evidence-based medicine helps hospitals maintain high-quality standards, leading to better patient satisfaction, fewer readmissions, and a reduced likelihood of malpractice suits. As a result, hospitals with strong faculty involvement often see improved financial performance due to more efficient care delivery and fewer complications.
- Cost Reduction Through Training and Innovation: Faculty members play a crucial role in educating medical students, residents, fellows, and other healthcare professionals. Their teaching fosters more effective, efficient, and cost-conscious care practices. This 24/7 training program not only improves the competence of future healthcare providers but can also help reduce unnecessary procedures, cuts down on hospital stays, and lower overall treatment costs … all of which improve the hospital’s financial bottom line.
- Research and Innovation: Many medical school faculty are engaged in research that drives innovation, leading to breakthroughs in treatment methods, technology, and healthcare delivery. Hospitals benefit financially from research funding, patents and other intellectual property, and the reputation boost that comes from being associated with pioneering work. This innovation, particularly in cutting-edge treatments and healthcare technology, can also attract a broader patient base and open new avenues of revenue.
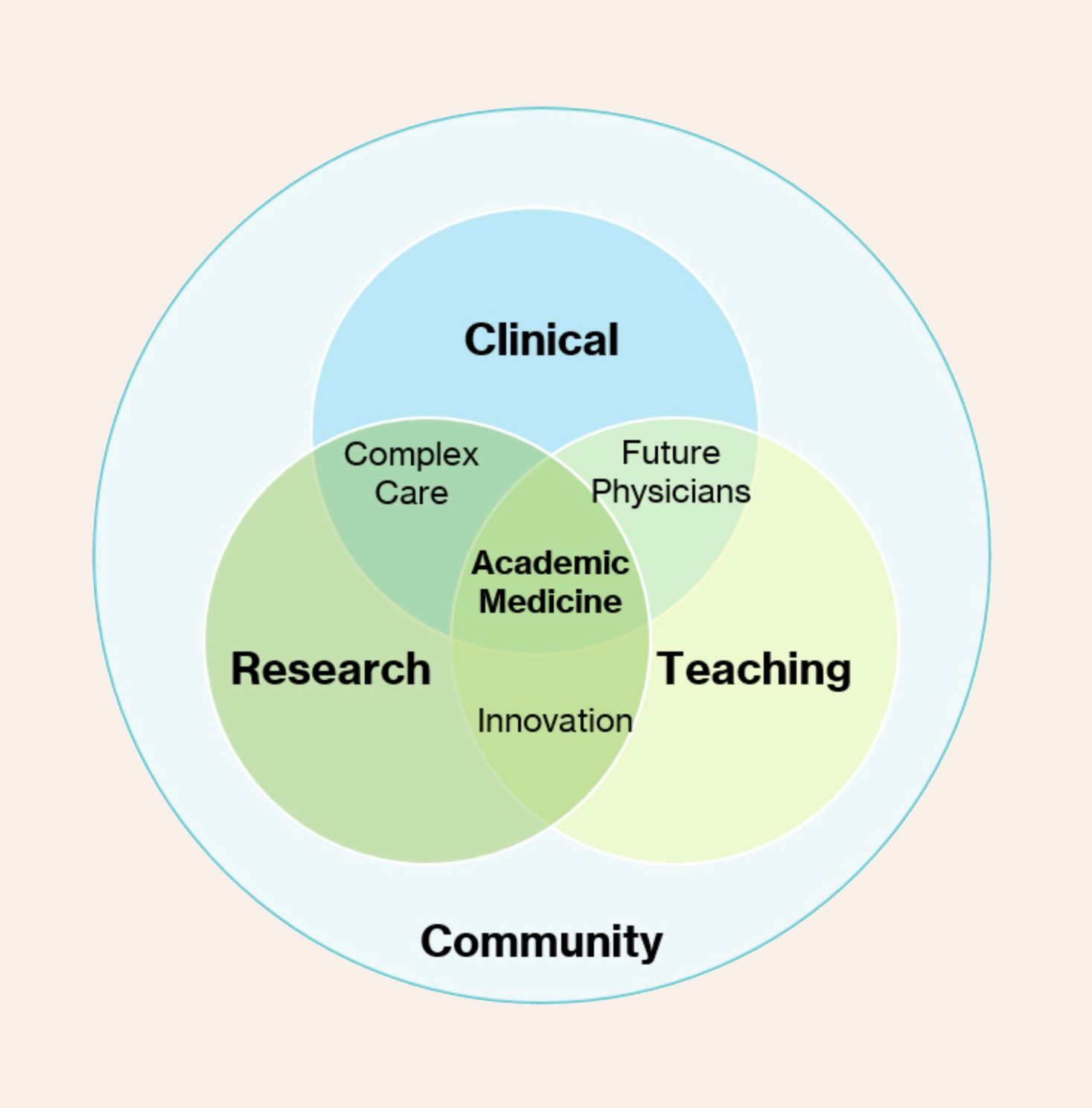
The financial relationship between a medical school and its teaching hospital is complex, but certain models can support long-term sustainability and growth for both institutions. These models are designed to balance costs, funding streams, and patient care needs.
Similarly, the tripartite mission of the medical school is dependent on a financially and operationally stable teaching hospital in several important ways as the medical school cannot function clinically, train future clinicians, or develop innovative clinical practices through research without the hospital. This interdependence will be explored in part 2 of this blog:
As the healthcare landscape continues to evolve, managing the flow of funds (and sharing of appropriate costs) between medical schools and teaching hospitals is more crucial than ever. The next step in ensuring long-term financial sustainability is developing more transparent and adaptable funding mechanisms that account for changes in healthcare delivery, research, and patient care needs. Through collaborative financial models and strategic partnerships, medical schools and teaching hospitals can continue to grow, providing cutting-edge care while fostering the next generation of healthcare professionals. The key to long-term success lies in balancing financial sustainability with the high standards of education and patient care that these institutions are committed to delivering, and the economic contribution analysis is the first step in quantifying each entity’s value of this critical partnership.
